
Prostate health index is useful for prostate cancer detecting in Chinese people
Introduction
Prostate cancer (PCa) incidence was increased substantially in the last two decades in China (1,2). Different from Western countries, more high-grade PCa (Gleason score 7 or more) were detected at the first time of diagnosis in Chinese. And un-similar with Western countries, total prostate specific antigen (tPSA) were higher than 10 ng/mL in most of those people (1,3-5).
For PCa detecting, total PSA was still an excellent biomarker now days, however tPSA was not PCa specific, other non-cancer conditions such as enlarged prostate and inflammation in the prostate may also lead to elevated PSA levels, so its specificity was relatively low, meanings a high prevalence of unnecessary biopsies (6-8).
To preserve the benefit of early detection while reducing over-diagnose, new biomarkers would be welcome to increase the specificity of the PSA test (1,5-8). [-2]proPSA (p2PSA), a truncated PSA isoform, was demonstrated better accuracy than serum tPSA and fPSA in detecting PCa. The prostate health index (PHI), derived from a combination of p2PSA, tPSA, and fPSA (free PSA) had been shown to be better predictor of PCa (9-14), had been approved by the United States Food and Drug Administration (FDA) and the European Medicines Agency (EMA). There were many papers reported the PHI is a better predictor of PCa in patients from Europe and American (1,6,10,12-14), but few papers in Chinese people. In this paper, we would using an observational prospective study design to test whether PHI could aid in clinical practice.
Methods
Patients and tissue samples
A total of 108 consecutive patients which visited doctors between 2014 and 2016 in No. 1 affiliated Hospital of Soochow University were included in this study. After written informed consent, PHI and PSA was detected for each patient before any study-specific investigation was performed. Transrectal ultrasound (TRUS)-guided biopsy was performed using a 12-core scheme. All biopsy specimens were reviewed by two doctors at the Pathology Department. This study was approved by the ethic committees at local hospitals.
Laboratory methods
Beckman Coulter’s DxI800 Immunoassay System was using to detecting Serum p2PSA, tPSA and fPSA of each patient. PHI was calculated by ([p2PSA/fPSA]×. Performance of individual PSA and PHI measurements in discriminating clinical outcomes was measured using the detection rate of PCa, sensitivity, specificity, and the area under the receiver operating characteristic curve (AUC) (1,6).
Statistical analysis
Statistical analyses were conducted using the Statistical Package of the Social Sciences software version 19.0 (SPSS, Inc.). A two-sided P<0.05 was considered to be statistically significant.
Results
A total 108 patients were recruited in this research. Baseline characteristic of all patients were shown in Table 1. Most of the patients were aged between 60 and 70 years, mean of all patients age was 69.4 [47–87] years.
Table 1
| Characteristics | Overall, n=108 | Absence of PCa, n=57 (52.8%) | Presence of PCa, n=51 (47.2%) | P value |
|---|---|---|---|---|
| Age, yr | 69.4±6.8 [47–87] | 68.9±7.4 | 69.9±6.2 | >0.05 |
| tPSA, ng/mL | 20.6±4.24 (2.23–149) | 10.3±8.4 | 30.3±38.4 | <0.05 |
| fPSA, ng/mL | 2.88±4.2 (0.03–20) | 1.9±1.6 | 3.8±5.6 | >0.05 |
| PHI | 142.8±340.8 (6.85–2,986.2) | 46.5±17.5 | 233.2±458.2 | <0.05 |
PCa, prostate cancer; tPSA, total prostate specific antigen; fPSA, free prostate specific antigen; PHI, prostate health index.
Among all people, 51 patients were diagnosed with PCa, 57 patients were absence of PCa, mean of age in PCa group is 69.9, while in absence of group it is 68.9. fPSA was 3.8 vs. 1.9 ng/mL. No different with age and fPSA. PHI and tPSA were higher in PCa group, in the group of absence of PCa, mean of tPSA was 10.3 ng/mL, in PCa group was 30.3 ng/mL (P<0.05). Similar as tPSA, PHI was higher in PCa group, in PCa group, mean of PHI was 233.2 ng/mL, while in absence of PCa, there was 46.5 ng/mL only (P<0.05).
To get the more effect marker in predicted PCa, the PHI, PHI + tPSA and tPSA were selected. When we choose 60% sensitivity, the specificity for PSA to detect PCa was 68%, while the PHI and tPSA + PHI was 86%, 87.7% respect. When sensitivity was 70%, the specificity of PSA was 56.1%, PHI and tPSA + PHI were decrease to 75.4% and 77.2%. With 80% sensitivity, the specificity of PSA was 38.6%, PHI and PHI + PSA were 45.6% (Table 2). All that means the specificity of PHI or PHI + PSA were higher than PSA.
Table 2
| Sensitivity (%) | Specificity (%) |
|---|---|
| 60 | |
| tPSA | 68.0 (54.8–80.1) |
| PHI | 86.0 (74.2–93.7) |
| tPSA + PHI | 87.7 (76.3–94.9) |
| 70 | |
| tPSA | 56.1 (42.4–69.3) |
| PHI | 75.4 (62.2–85.9) |
| tPSA + PHI | 77.2 (64.2–87.3) |
| 80 | |
| tPSA | 38.6 (26–52.4) |
| PHI | 45.6 (32.4–93.7) |
| tPSA + PHI | 45.6 (32.4–93.7) |
tPSA, total prostate specific antigen; fPSA, free prostate specific antigen; PHI, prostate health index.
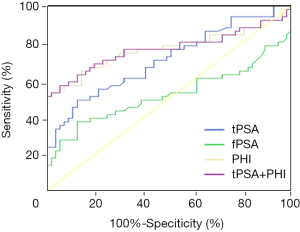
Compared with tPSA measurement, AUC was always higher for PHI. In detecting PCa, AUC of PHI was 76.6%, tPSA + PHI was 76.7%, while tPSA was only 70.8% (compare with 50%, P<0.05), the difference of AUC between PHI and PSA was about 6% in the entire cohort (Figure 1).
We also evaluated the benefit of PHI over tPSA in reducing the number of biopsies. As Table 3 show, in 57 PCa negative patients, there were 37 patients need to do biopsies with the cutoff value of tPSA >4 ng/mL; while with the value of PHI >40, only 30 patients need do. Seven patients could avoid unnecessary biopsies. When combined with the two values (tPSA >4 ng/mL, PHI >40) only 24 patients remained (P<0.05).
Table 3
| tPSA (ng/mL) | PHI | |
|---|---|---|
| ≤40 | >40 | |
| ≤4 | 14 | 6 |
| >4 | 13 | 24 |
tPSA, total prostate specific antigen; PHI, prostate health index.
Discussion
Although reasons were unclear, the PCa incidence and its trend were differences in Western countries and China. The incidence in China was lower than Western counties. More PCa patients in first diagnosed were high-grade PCa in China compared with Western country. Furthermore, the gray zone is different in Chinese patients from Western country (2,6,15). So some useful marker in detecting PCa in Western country need to validated in Chinese people, such as PHI. Derived from a combination of p2PSA, tPSA, and fPSA, PHI had been shown to be a better predictor of PCa in Western country. Similar as the results of Western country, we find that PHI performed better than tPSA in PCa detecting. The specificity of PHI and PHI + tPSA is higher than tPSA. The PHI achieved an AUC 76.7% while tPSA was 70.8%. All those date meanings that PHI-based strategy can reduce the number of unnecessary biopsies while maintaining the same detection rate of PCa.
Although additional muti-center with larger sample size need, our results identified the PHI can be used as a new reference standard for PCa detecting in China.
Acknowledgments
We thank Jingxian Pu, Jun Ouyang, Gang Li, Chunying Yan, Hexing Yuan, Xiang Ding for making this study possible.
Funding: Research supported partially by grants from
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/tcr.2019.05.08). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). The institutional research ethics committee approved the experimental protocols. Informed consent was obtained from all patients.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Zhu Y, Han CT, Zhang GM, et al. Development and external validation of a prostate health index-based nomogram for predicting prostate cancer. Sci Rep 2015;5:15341. [Crossref] [PubMed]
- Zhu Y, Wang HK, Qu YY, et al. Prostate cancer in East Asia: evolving trend over the last decade. Asian J Androl 2015;17:48-57. [Crossref] [PubMed]
- Cullen J, Elsamanoudi S, Brassell SA, et al. The burden of prostate cancer in Asian nations. J Carcinog 2012;11:7. [Crossref] [PubMed]
- Ankerst DP, Boeck A, Freedland SJ, et al. Evaluating the PCPT risk calculator in ten international biopsy cohorts: results from the Prostate Biopsy Collaborative Group. World J Urol 2012;30:181-7. [Crossref] [PubMed]
- Ren S, Xu J, Zhou T, et al. Plateau effect of prostate cancer risk-associated SNPs in discriminating prostate biopsy outcomes. Prostate 2013;73:1824-35. [Crossref] [PubMed]
- Na R, Ye D, Liu F, et al. Performance of serum prostate-specific antigen isoform [-2]proPSA (p2PSA) and the prostate health index (PHI) in a Chinese hospital-based biopsy population. Prostate 2014;74:1569-75. [Crossref] [PubMed]
- Kirby RS, Fitzpatrick JM, Irani J, et al. Prostate cancer diagnosis in the new millennium: strengths and weaknesses of prostate-specific antigen and the discovery and clinical evaluation of prostate cancer gene 3 (PCA3). BJU Int 2009;103:441-5. [Crossref] [PubMed]
- Bjartell A. PSA and prostate cancer screening: the challenge of the new millennium. Eur Urol 2007;52:1284-6. [Crossref] [PubMed]
- Jansen FH, van Schaik RH, Kurstjens J, et al. Prostate-specific antigen (PSA) isoform p2PSA in combination with total PSA and free PSA improves diagnostic accuracy in prostate cancer detection. Eur Urol 2010;57:921-7. [Crossref] [PubMed]
- Stephan C, Vincendeau S, Houlgatte A, et al. Multicenter evaluation of [-2]proprostate-specific antigen and the prostate health index for detecting prostate cancer. Clin Chem 2013;59:306-14. [Crossref] [PubMed]
- Ferro M, Bruzzese D, Perdona S, et al. Predicting prostate biopsy outcome: Prostate health index (phi) and prostate cancer antigen 3 (PCA3) are useful biomarkers. Clin Chim Acta 2012;413:1274-8. [Crossref] [PubMed]
- Ferro M, Bruzzese D, Perdona S, et al. Prostate Health Index (Phi) and Prostate Cancer Antigen 3 (PCA3) significantly improve prostate cancer detection at initial biopsy in a total PSA range of 2–10 ng/mL. PLoS One 2013;8:e67687. [Crossref] [PubMed]
- Filella X, Foj L. Prostate Cancer Detection and Prognosis: From Prostate Specific Antigen (PSA) to Exosomal Biomarkers. Int J Mol Sci 2016;17:E1784. [Crossref] [PubMed]
- Filella X, Foj L, Auge JM, et al. Clinical utility of %p2PSA and prostate health index in the detection of prostate cancer. Clin Chem Lab Med 2014;52:1347-55. [Crossref] [PubMed]
- Na R, Jiang H, Kim ST, et al. Outcomes and trends of prostate biopsy for prostate cancer in Chinese men from 2003 to 2011. PLoS One 2012;7:e49914. [Crossref] [PubMed]


